Myelofibrosis Symptoms, Causes, Diagnosis and Treatment
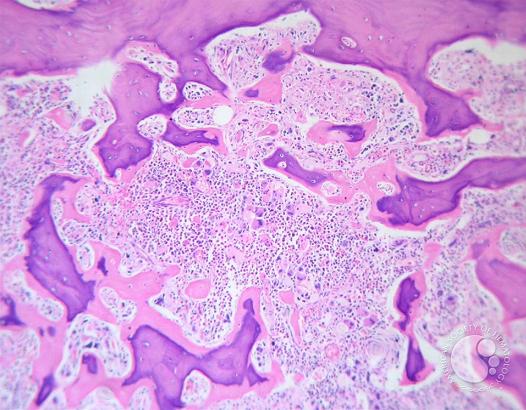
What Is Myelofibrosis?
It is a life-threatening bone marrow disorder which disturbs the normal growth of blood cells in a body. Such tends to consequent scarring in the bone marrow, causing weakness, anemia and enlarged liver and spleen. The disorder is a rare form of chronic leukemia, and belongs to a diseases group named myeloproliferative disorders. Typically, the condition of individuals suffering from myelofibrosis gradually worsens, where few ultimately develops a more acute type of leukemia.
One may have myelofibrosis for years without any prominent symptoms. Its treatment aims to ease the symptoms.
What Are The Symptoms Of Myelofibrosis?
Usually, the disorder advances gradually. In its initial stages, many individuals do not notice any signs, however as it increasingly interferes with the normal production of blood cells with the passage of time, symptoms begins more and more apparent, they may include:
- Fever.
- Night sweats.
- Bone pain.
- Frequent infections.
- Easy bleeding.
- Easy bruising.
- Pale skin.
- Fullness or pain under the ribs on your left side, because of enlarged spleen.
- Feeling weak and tires.
- Breathing difficulties due to anemia.
What Causes Myelofibrosis?
Developing genetic mutation in the stem cells of blood causes myelofibrosis. Normally, these stem cells replicate and split into many specialized cells which compose our blood-platelets, white blood cells and red blood cells. What exactly grounds genetic mutation, is still a mystery.
What Are The Risk Factors Of Myelofibrosis?
Even though, what exactly triggers the bone marrow disorder is unknown till date, however few factors are considered to increase its chances:
- Older adults between the ages of 50-60 are more likely to experience myelofibrosis.
- Specific chemical exposure for example benzene and toluene.
- High levels of radiation exposure.
What Are The Potential Complications Of Myelofibrosis?
Certain complications linked with myelofibrosis include:
- Back pain and abdominal pain due to an enlarged spleen.
- Raised pressure on the blood flowing into the liver.
- Growth in some other body parts.
- Bleeding complications.
- Painful joints and bones.
- Gout.
- Acute leukemia.
How Is Myelofibrosis Diagnosed?
In order to diagnose myelofibrosis, the doctor can suggest the following procedures and tests:
- Physical exam.
- Blood tests.
- Imaging tests.
- Bone marrow examination.
- Gene tests.
How Is Myelofibrosis Treated?
An identified curative treatment of myelofibrosis is allogeneic stem cell transplantation, though; the treatment tends to involve potential risks. Few other treatment options of the bone marrow disorder are highly supportive and include:
- Blood transfusions.
- Allopurinol.
- Regular folic acid.
Few other treatment options such as hydroxyurea, alpha-interferon and dexamethasone also play a major role for treating the bone marrow disoder.
Thalidomide and lenalidomide are also used for treating myelofibrosis, however they share a common side-effect, peripheral neuropathy. Frequent blood transfusion is often needed by the patient of myelofibrosis. Lastly, ruxolitinib, is another latest treatment option approved for myelofibrosis.
By : Natural Health News




